Eye Movement Desensitization and Reprocessing (EMDR) therapy is a form of psychotherapy designed to reduce distress associated with traumatic memories.
The goal of EMDR is to help individuals process and overcome experiences that are causing post-traumatic, anxiety, or depressive symptoms.
It aims to promote the mind’s natural healing capacity using bilateral stimulation and guided processing of traumatic memories.

In an EMDR session, the client focuses on traumatic images, negative thoughts, emotions, or sensations while simultaneously moving their eyes back and forth tracking the therapist’s fingers or a light bar.
This bilateral stimulation is believed to mimic rapid eye movement (REM) sleep and facilitate neurological reprocessing of memories for healing and adaptive relief from symptoms.
EMDR therapy typically takes 6-12 sessions over the course of several weeks.
Research indicates it can rapidly reduce symptoms and outperforms other therapies in some contexts.
Beyond PTSD, EMDR is also used to address panic disorders, depression, dissociation, chronic pain, and more.
According to Megan Boardman, LCSW, author of The EMDR Workbook for Trauma and PTSD:
“The brain’s information processing system naturally moves toward mental health. If the system is blocked or imbalanced by the impact of a disturbing event, the emotional wound festers and can cause intense suffering. Once the block is removed, healing resumes.”
How was EMDR developed?
EMDR was initially developed by Francine Shapiro in 1987. She found that when thinking about her own trauma, she would move her eyes from side to side and found that this helped reduce the occurrence of distressing memories.
EMDR was officially introduced as a therapy by Shapiro in 1989 for treating traumatic memories. It has since been proposed for various anxiety disorders, such as PTSD, panic disorder, and specific phobias.
Although a relatively new type of psychotherapy, EMDR has become widely used and is an effective treatment for many conditions, especially trauma-related.
EMDR is guided by the Adaptive Information Processing model. The model proposes that the symptoms of PTSD and other disorders (unless physically or chemically caused) result from past disturbing experiences that continue to cause distress because the memory was not processed.
The unprocessed memories are understood to contain the emotions, thoughts, beliefs, and physical sensations that occurred during the traumatic event.
Essentially, traumatic and painful memories can cause distressing emotions when they are unprocessed.
Adaptive Information Processing
The theoretical basis of EMDR is rooted in the Adaptive Information Processing (AIP) model, which views psychological dysfunction as emerging from unprocessed memories stored in maladaptive neural networks (Russell & Shapiro, 2022).
These dysfunctional networks drive perceptions and reactions to current experiences. EMDR aims to forge connections between these problematic networks and existing adaptive networks containing memories of mastery, resilience and growth.
In this way, distressing memories can be linked to more positive associations and restored in an adaptive form.
A core assumption is that the brain has an innate capacity to process adversity toward resolution. EMDR seeks to activate this self-healing mechanism through dual-focused attention and bilateral stimulation.
The Eight Phases of EMDR Therapy
EMDR therapy is an eight-phase treatment. Eye movements (or other bilateral stimulation) are used during part four of the treatment.
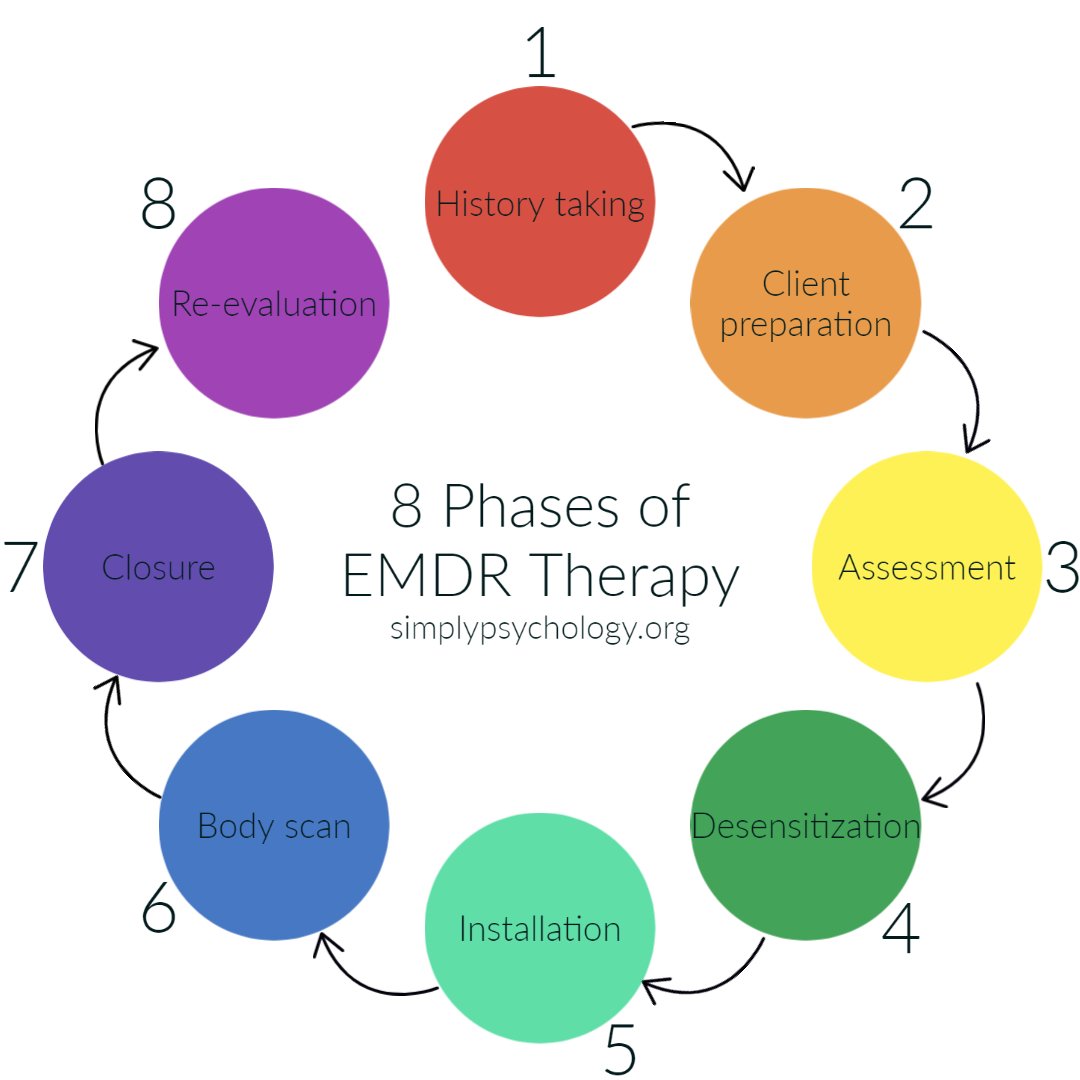
With EMDR, the client typically has one or two weekly sessions for around 6-12 weeks. There are eight phases to EMDR, which will be detailed below:
Phase 1: History taking
The first step in EMDR is to review the client’s symptoms and health history to understand better where they are in the treatment process.
In addition to getting a full health history and conducting appropriate assessments, the therapist and client work together to identify targets for treatment. These targets can include looking at memories, current triggers, and future goals.
These evaluation phases also include briefly discussing the trauma and identifying potential memories that can be addressed.
Phase 2: Client preparation
To prepare the client for the therapy, the therapist will teach a few different techniques to help the client to manage and cope with their emotional distress or uncomfortable feelings that may come up during treatment.
This is known as resourcing. Finding the right stress management technique that works for the client can take some time. They may be asked to try several techniques, and perhaps only one or two work for them.
The therapist will explain the reasons for the treatment and introduce the client to the procedures, practicing eye movements and/or other bilateral stimulation components to ensure they can carry this out.
Phase 3: Assessment
The therapist will then guide the client through selecting a specific memory to target, along with any relevant aspects of the memory, such as painful emotions, physical sensations, intrusive thoughts or images, and distressing self-beliefs.
This will all help to activate the memory that is being targeted in the session.
Two measures are used to evaluate changes in emotion and cognition: the Subjective Units of Disturbance (SUD) scale and the Validity of Cognition (VOC) scale. Both measures are used again during the treatment process in accordance with the standardized procedures.
For the VOC scale, the therapist may ask the client: ‘When you think of the incident, how true do those words feel to you now on a scale of 1-7, where 1 feels completely false, and 7 feels totally true?’
After the client has named the emotions they are experiencing, the therapist may use the SUD scale to ask: ‘On a scale of 0-10, where 0 is no disturbance or neutral and 10 is the highest disturbance you can imagine, how disturbing does it feel now?’
The therapist will then begin using EMDR techniques to address the targeted memories in four stages (Phases 4-7).
Phase 4: Desensitization
During the desensitization phase, the client will be encouraged to focus on the memory, thought, or image while engaging in eye movements or other bilateral stimulation.
The bilateral stimulation may involve tapping, audio tones, blinking lights, or left-to-right activation.
The client will then be asked to let their mind go blank and notice any thoughts and feelings spontaneously coming up. After each set of bilateral stimulation, the therapist will likely ask the client to share any thoughts, sensations, or images that came up during the set.
After these thoughts have been identified, the therapist may have the client refocus on that traumatic memory or move on to another if that memory no longer triggers unwanted emotions.
The process will continue until the client reports that the memory is no longer distressing.
Phase 5: Installation
This phase will involve the client ‘installing’ a positive self-belief or image to replace the unwanted belief they identified in phase 3.
The focus of this phase is to strengthen the preferred positive cognition. The client will focus on this new belief through another repetition of bilateral stimulation.
Phase 6: Body scan
The client will be asked to ‘scan’ their body while thinking of the memory and the positive cognition. They will be encouraged to identify any somatic distress that may still be residing in their body.
If there is still some disturbance, standardized procedures involving bilateral stimulation will be used to process this.
Phase 7: Closure
At the end of each session, the therapist will explore the client’s progress and suggest relaxation techniques and other coping strategies they can use between sessions to help maintain improvements.
If the targeted memory was not fully processed in the session, specific instructions are given to provide containment and ensure safety until the next session.
Phase 8: Re-evaluation
The next therapy session will start at phase 8, during which the therapist evaluates the client’s current psychological state and observes whether the effects from the previous session have lasted.
The therapist and the client will also go through what memories may have emerged since the last session and identify targets for the current session.
Coping Strategies
Stress reduction techniques can help manage the client’s emotions during and between sessions, including breathing exercises and resourcing techniques.
Resourcing refers to identifying and instilling coping skills to help deal with difficult reactions. Resourcing can be used anytime disturbing emotions, thoughts, images, and/or physical sensations are experienced.
Some techniques may work better than others, but clients can choose their go-to resource during EMDR sessions or between sessions. Some examples of resourcing include:
Butterfly hug
This technique involves having the arms crossed over the chest, with hands and fingers being as vertical as possible, possibly interlocking the thumbs if this helps.
Next, alternate the hand movement, which signifies a butterfly’s flapping wings.
While doing this, breathe slowly and deeply while observing what is going through the mind and body, such as thoughts, images, sounds, smells, and feelings, without pushing the thoughts away or judging them.
Safe/calm/healing place
While having your eyes closed and using your imagination, go to a place that feels safe or calm.
While concentrating on the pleasant sensations in the body, the therapist will use bilateral stimulation to strengthen the association of the positive experience with the place.
Container
This technique works by imagining a container to store upsetting thoughts, feelings, and images. The container needs to have a way to add and remove memories, thoughts, and images, as well as be able to regulate how much comes out at any one time.
To test if this resource is helpful, consider a slightly disturbing experience, bring up the container and notice any shifts in the body. Then, picture putting this experience and any associated feelings into the container.
Coherent breathing
When inhaling and exhaling, engage the diaphragm rather than breathing from the chest and shoulders. Think about the diaphragm as a balloon that can be expanded on the inhale and decompressed on the exhale.
The ideal breath rate is about six breath cycles per minute. The heart and brain should be more balanced and calm at this breath rate.
Mindfulness
Mindfulness is a type of meditation focused on being intensely aware of what is being sensed and felt at the present moment.
Mindfulness also involves acceptance, meaning that attention is paid to thoughts and feelings without judging them or believing there is a right or wrong way to think or feel in a given moment.
Benefits of EMDR
There are many reasons why someone may consider EMDR therapy.
While EMDR may not work for everyone, there are some main ‘selling points’ that this type of therapy promotes. These can include the following:
Reducing negative thinking
EMDR therapy can help to identify and challenge any negative thoughts associated with the distressing memory.
For instance, someone may look back on their traumatic memory and believe that they were fully at fault for what happened, even if this was not true.
EMDR can help declutter the mind of these negative thoughts and replace them with more helpful and positive ones.
Unlike talk therapy,the insights clients gain in EMDR therapy result not so much from clinician interpretation, but from the client’s own accelerated intellectual and emotional processes.
Rapid results
The main selling point of EMDR therapy is that it tends to yield faster results than other psychotherapies.
While it is not helpful to expect to complete the therapy as quickly as possible- since some clients may need extra sessions- many people who undergo EMDR report positive results within as little as three sessions.
Unlike other treatments that focus on altering the emotions, thoughts, and responses resulting from the traumatic experiences, EMDR focuses directly on the memory, which causes distressing feelings.
This may be why EMDR can be a quicker treatment than other therapies, as it helps with the root cause of the distress.
Minimal talking
In EMDR therapy, there is no pressure to discuss all the details of a traumatic experience. Other talk therapies may involve going into the details to make the therapy effective.
Since there is little talking involved, EMDR may be helpful for people who have difficulty talking about their trauma.
Increase self-worth
As EMDR targets distressing memories and negative thoughts about the client, such as thoughts that they are weak, powerless, or useless, these thoughts can be changed.
Changing these negative thoughts about the self into something more positive can greatly impact the client’s self-esteem and confidence in themself.
How effective is EMDR?
EMDR has proven to be an effective therapeutic treatment method.
According to the EMDR Research Foundation, EMDR therapy has been clinically validated by more than 30 randomized controlled studies, which is the gold standard for clinical studies.
What does the research say?
-
According to the EMDR Institute, some studies for EMDR effectiveness show that 84%-90% of single-trauma victims no longer have PTSD symptoms after only three sessions.
-
A study compared the effectiveness of EMDR to cognitive behavioral therapy (CBT) in treating the symptoms of panic disorder and improving patients’ quality of life. The results determined that EMDR is just as effective as CBT (Horst et al., 2017).
-
The effectiveness of EMDR and trauma-focused CBT (TF-CBT) for posttraumatic stress symptoms was explored through met analyses. The results indicated that both therapies effectively treat these symptoms, but TF-CBT was marginally more effective (Lewey et al., 2018).
-
A study compared EMDR with CBT in children with behavioral problems. Both therapies were found to have significant positive effects on behavioral and self-esteem problems. Although the differences between the effects were small, children who received EMDR therapy showed significantly larger changes in target behaviors than those in the CBT group (Wanders et al., 2008).
-
A 2014 study looked at 24 randomized controlled trials that support the effectiveness of EMDR for the treatment of trauma. The results of some of these studies suggested that EMDR therapy is more effective than CBT for trauma (Shapiro, 2014).
-
A small pilot study found that EMDR was safe and effective in treating PTSD in people with a psychotic disorder (van den Berg & van der Gaag, 2012).
-
A small 2015 study reported that people who underwent EMDR treatment for depression were less likely than those in the control group to experience relapse or problems relating to depression in the year following treatment (Hase et al., 2015).
-
A review of studies on the effectiveness of EMDR found evidence that it may even help improve other non-traumatic symptoms found in mood disorders, as well as showing potential as an additional treatment for those with chronic pain (Valiente-Gómez et al., 2017)
-
A 2021 study surveyed data from 33 EMDR therapists who gave therapy online. The results showed that EMDR provided over the internet was shown to help still relieve mental health symptoms as it does in person (McGowan et al., 2021).
Future Directions for EMDR
Despite EMDR’s substantial evidence base and growth, further research and developments would benefit the field.
Additional RCTs are needed on diverse issues, including early interventions, treatment mechanisms, effectiveness in clinical practice, and delivery via telehealth (Lenferink et al., 2020).
Comparative dismantling studies between EMDR and other therapies could provide greater clarity on distinct change processes. There is also a need for more neuroimaging research on EMDR’s effects on brain structure and functioning.
Moreover, increased teaching of EMDR in university graduate programs would likely reduce lingering controversy and increase equitable access. This requires professional EMDR associations to expand trainer eligibility beyond approved programs.
Further cultural adaptations and implementation studies with marginalized groups are essential to expand EMDR’s clinical and preventative utility across cultural contexts.
Overall, advancing research on EMDR’s flexibility, efficiency, and mechanisms while proliferating high-quality training opportunities, will support this evidence-based psychotherapy reaching its fullest potential (Russell & Shapiro, 2022).
Things to consider
EMDR is generally recognized as a safe treatment, typically causing fewer adverse reactions than medications for trauma symptoms.
Unlike some medications, EMDR may maintain effectiveness after treatment ends since it deals with the root cause of distress.
Even so, EMDR, like other psychotherapies, may come with some side effects:
-
An increase in distressing memories.
-
It can feel very exhausting after the first session while you bring up traumatic memories that may have been pushed down for a long time.
-
Heightened emotions or physical sensations during sessions that may last beyond the session.
-
Light-headedness.
-
Some more report unpleasant or vivid dreams while they begin to reprocess traumatic events.
-
The surfacing of new traumatic memories if EMDR is not used appropriately.
Despite this, symptoms of new emotions or physical sensations typically resolve as the treatment continues. Ensure you work with the therapist to find ways to cope with your feelings as you go forward with therapy.
If you become distressed during therapy, your therapist will help you to return to the present before shifting to another traumatic memory.
It is important to discuss all considerations with a medical professional before choosing to undergo EMDR therapy.
Further Information
Shapiro, F. (1995). Eye movement desensitization and reprocessing.
References
Hase, M., Balmaceda, U. M., Hase, A., Lehnung, M., Tumani, V., Huchzermeier, C., & Hofmann, A. (2015). Eye movement desensitization and reprocessing (EMDR) therapy in the treatment of depression: a matched pairs study in an inpatient setting. Brain and Behavior, 5 (6), e00342.
Horst, F., Den Oudsten, B., Zijlstra, W., de Jongh, A., Lobbestael, J., & De Vries, J. (2017). Cognitive behavioral therapy vs. eye movement desensitization and reprocessing for treating panic disorder: a randomized controlled trial. Frontiers in Psychology, 8, 1409.
Lenferink, L. I., de Keijser, J., Smid, G. E., & Boelen, P. A. (2020). Cognitive therapy and EMDR for reducing psychopathology in bereaved people after the MH17 plane crash: Findings from a randomized controlled trial. Traumatology, 26(4), 427.
Lewey, J. H., Smith, C. L., Burcham, B., Saunders, N. L., Elfallal, D., & O’Toole, S. K. (2018). Comparing the effectiveness of EMDR and TF-CBT for children and adolescents: A meta-analysis. Journal of Child & Adolescent Trauma, 11( 4), 457-472.
Mazzei, R. (2021, January 27). What is Resourcing in EMDR Therapy? Evolutions Behavioral Health Services. https://www.evolutionsbh.com/articles/what-is-resourcing-in-emdr-therapy/
McGowan, I. W., Fisher, N., Havens, J., & Proudlock, S. (2021). An evaluation of eye movement desensitization and reprocessing therapy delivered remotely during the Covid–19 pandemic. BMC psychiatry, 21 (1), 1-8.
Russell, M. C., & Shapiro, F. (2022). Eye movement desensitization and reprocessing (EMDR) therapy. American Psychological Association. https://doi.org/10.1037/0000273-000
Shapiro, F. (1989). Eye movement desensitization: A new treatment for post-traumatic stress disorder. Journal of behavior therapy and experimental psychiatry, 20(3), 211-217.
Shapiro, F. (2014). The role of eye movement desensitization and reprocessing (EMDR) therapy in medicine: addressing the psychological and physical symptoms stemming from adverse life experiences. The Permanente Journal, 18 (1), 71.
Shapiro, F. (2017). Eye movement desensitization and reprocessing (EMDR) therapy: Basic principles, protocols, and procedures. Guilford Publications.
Shapiro, F., & Maxfield, L. (2002). Eye movement desensitization and reprocessing (EMDR): Information processing in the treatment of trauma. Journal of clinical psychology, 58 (8), 933-946.
Valiente-Gómez, A., Moreno-Alcázar, A., Treen, D., Cedrón, C., Colom, F., Perez, V., & Amann, B. L. (2017). EMDR beyond PTSD: A systematic literature review. Frontiers in psychology, 8, 1668.
van den Berg, D. P., & van der Gaag, M. (2012). Treating trauma in psychosis with EMDR: a pilot study. Journal of behavior therapy and experimental psychiatry, 43 (1), 664-671.
Wanders, F., Serra, M., & De Jongh, A. D. (2008). EMDR versus CBT for children with self-esteem and behavioral problems: A randomized controlled trial. Journal of EMDR Practice and Research, 2 (3), 180-189.

